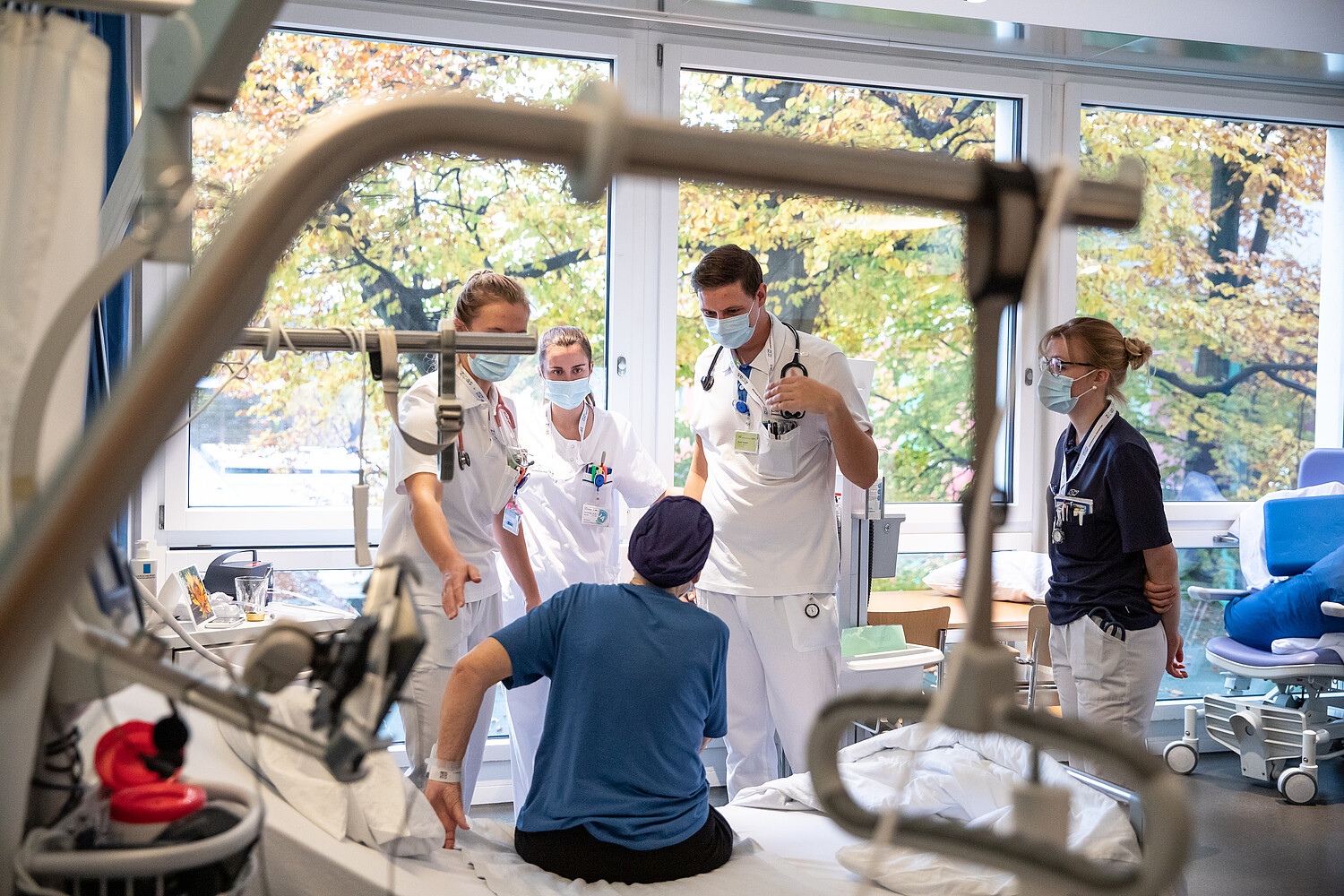
ZIPAS: When students treat sick people by themselves
At the Kantonsspital Winterthur, trainees and students from several healthcare professions jointly manage two patient rooms. The ZIPAS training model increases their awareness of vital interprofessional collaboration.
“There’s a bit of rattling”, medical student Sophie Strasser tells the patient in the hospital bed. “You still have a little water in your lung.” Not only the aspiring doctor, but also a nursing student and a future physiotherapist listen to the elderly woman with a stethoscope. After their ward round, they compare notes in the corridor. Sophie Strasser finally decides to increase the dose of the medicine used to treat the woman’s pulmonary oedema. “Let’s see if that brings further improvement”, she says. “We are a motivated team”, she says later, as she writes a report in the ward’s office. “We share our knowledge with one another.”
“We work together as equals and benefit from each other.”
This is what the ZIPAS training model (see box) aims to achieve. Zipas stands for Zurich interprofessional clinical training ward. “The participants are meant to develop a better understanding of and openness towards other medical professional groups”, says Seraina Beerli, deputy director of vocational/occupational training at Kantonsspital Winterthur (KSW). “They should learn from and with one another.”
Exchanging ideas on an equal footing
At the beginning of November, when this report was written, seven students of medicine, nursing and physiotherapy were responsible for two rooms in the general medical department at KSW. They organise themselves and tend to patients independently. Three supervisors, known as facilitators, are on hand to provide support. “We work together as equals and benefit from each other”, says Lionel Fend, who is studying nursing at ZHAW Zurich University of Applied Sciences and is doing his final work placement. Among other things, he gained fascinating insights from the X-ray reports, which are otherwise accessible only to the medical fraternity. In return, he practised with the future doctors how to insert a venous catheter and take blood. “The nurses do that on a more routine basis than we do”, says Paula von der Lage, who is studying medicine at the University of Zurich. This morning, she’s assisting her colleague from physiotherapy with a walking training session. Together they walk with a patient down the long corridor and up a flight of stairs. On the way back, Paula takes over the task of supporting the elderly woman. “We deliberately hand over specific tasks to one another”, she says. This increases mutual appreciation for each other’s work.
Each team goes its own way

The keywords ‘appreciation’, ‘ability to handle conflict’ and ‘creativity’ can also be read on a pinboard in the office. These terms designate three interprofessional skills which the ZIPAS team is focusing on this week. At the end of their training stint, students are expected to have improved in twelve interprofessional skill areas. “The participants complement one another’s learning and develop together”, says Seraina Beerli. She has supervised two trial cohorts of the ZIPAS model at KSW, and is now happy with the regular operation of the model. Each group works differently, each goes its own way.
“I don’t present ideas; I ask questions.”
“The learners should be empowered to find a solution themselves”, says Facilitator Vanessa Vega, who works as a nursing care trainer at KSW. She deliberately stays in the background. “I don’t present ideas; I ask questions.” She steps in only if patient safety is at risk. For instance, she will point out that an antibiotic can be administered intravenously without flushing out the catheter first. “There’s always a certain risk of infection when flushing out”, she explains.
Staff and patients more satisfied

Facilitators are required to have a broad range of specialist knowledge and must stay on top of things, says Marion Huber from ZHAW’s faculty of healthcare. They have to accept creative solutions. “The participants learn by acting in a self-directed manner and reflecting on their actions.” In the ZIPAS Project group, Marion Huber headed the expert group that defined the learning objectives. In addition, the professor of ZHAW School of Health Professions provides academic supervision for the ZIPAS programme, and reports positive impacts. For instance, the interdisciplinary cooperation is associated with better workflows and shorter channels of communication. Bureaucracy is decreasing. Staff value the exchange and are motivated. Patients receive high-quality care and feel safe. On average, their stays in the hospital are shorter than is the case on similar wards. This tends to bring costs down.
“The participants learn by acting in a self-directed manner and reflecting on their actions.”
Seraina Beerli confirms these findings from day-to-day hospital life. “Patients are happy when they don’t have to answer the same questions over and over again.” There is less duplication. The participants are also positive. “We’ll leave here with the awareness and appreciation of other occupational groups”, says Lionel Fend. He thinks it would be good if all nursing students could have this sort of working experience.
“Mutual understanding is really valuable”, agrees Sophie Strasser. She appreciates being able to work autonomously and take responsibility as part of ZIPAS. She believes that patients and the healthcare system as a whole would benefit from more interconnectedness among the separate disciplines. Many experts emphasise that interprofessionalism needs to be strengthened, in view of rising costs, demographic trends and the shortage of specialists. “It can be an important building block in overcoming these challenges”, says ZIPAS Project leader Gert Ulrich from Careum. The KSW aims to place even more emphasis on the interprofessional approach in the future. The hospital envisages setting up ZIPAS wards in additional departments.
The ZIPAS model is the only scheme of its kind in Switzerland, and is arousing interest
Having trainees from different healthcare professions looking after clinical patients jointly and on an interprofessional basis is a new approach in Switzerland. University Hospital Zurich started ZIPAS in 2019. The hospital operates ZIPAS wards in its surgery and internal medicine departments. The first full run recently took place at Cantonal Hospital Winterthur. Pilot stages are currently running at Balgrist University Hospital and at Children’s Hospital Zurich. “We’ve already received inquiries from other cantons”, says Project leader Gert Ulrich. The ZIPAS concept is structured so that it can be expanded to other medical areas, departments and hospitals.
Six institutions worked together to develop the approach: the Careum Training Centre for health professions, the Careum Foundation, the University of Zurich Faculty of Medicine, University Hospital Zurich, the Centre for Healthcare Training and the School of Health Professions at ZHAW. The group took inspiration for the scheme from Sweden, where similar models have been in operation since the 1990s. Delegations from the ZIPAS Project group have visited clinics in Stockholm on two occasions. “In Zurich, we’ve opted for a broader, theory-based approach”, explains Ulrich. The Project team has put a lot of time and effort into getting to grips with the principles of the model. Among other things, the team defined learning objectives, created training plans, tested feasibility and evaluated pilot phases on an academic level. It has developed a manual from which other hospitals can now also benefit. “All six institutions contributed their expertise”, says Gert Ulrich. “This shared approach is innovative and productive.” It has resulted in ideas for other interdisciplinary collaborations within the ZIPAS Project group.
0 Comments
Be the First to Comment!